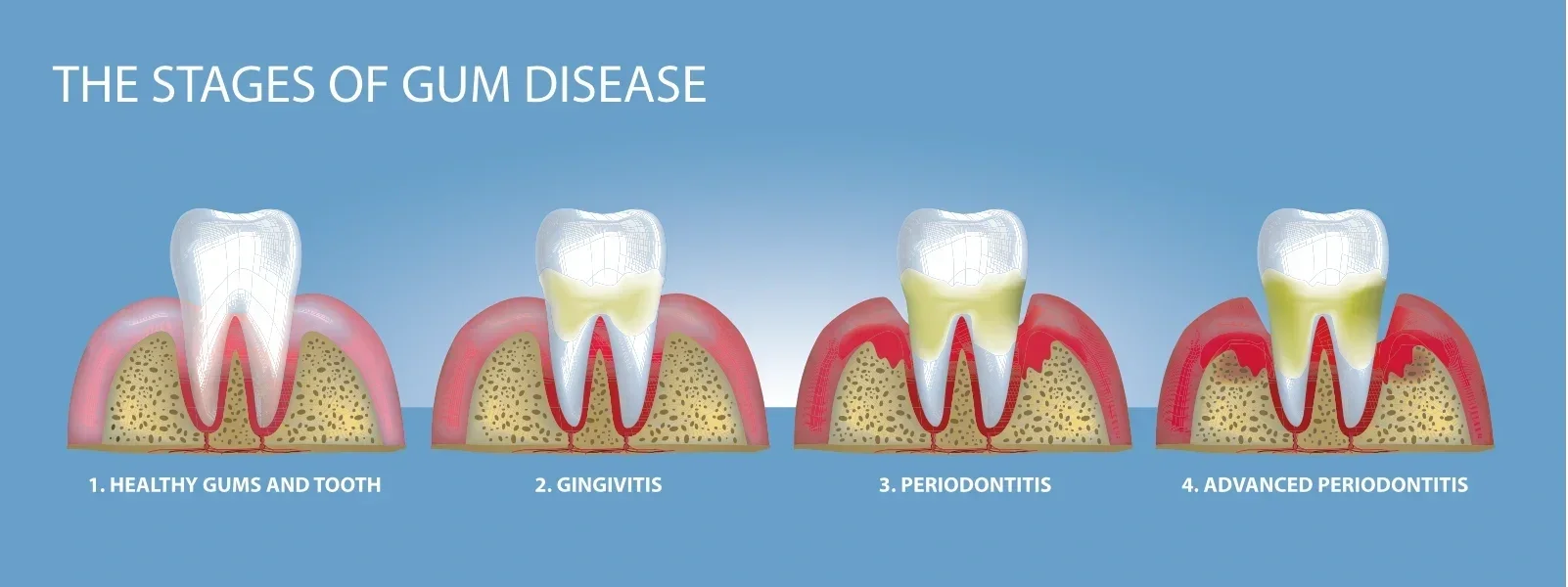
A periodontist is a dentist who specializes in the prevention, diagnosis, and treatment of periodontal disease (a chronic inflammatory disease that affects the gums and bone supporting the teeth also known as gum disease), and in the placement of dental implants.
Key concepts:
The oral cavity (the mouth) is the first part of the digestive tract.
Reflects the systemic health of an individual, and some individuals are at greater risk of oral health problems due to systemic health.
The digestive tract is full of bacteria.
Which bacteria and quantity of bacteria is reflected by our diet, our genetics, and particularly in our mouth --> Oral hygiene.
The oral cavity is unique within the digestive tract, such that these bacteria are separated from the systemic circulation by a mechanical barrier, as opposed to a cellular barrier throughout the remainder.
Mechanical barrier is unique, because once destroyed or damaged it cannot regenerate.
This barrier is located just below the edge of our gums surrounding our teeth and we must keep up good oral hygiene to preserve this delicate barrier.
Without adequate hygiene, we will see bleeding gums, and if not dealt with, this will progress to irreversible damage.
What is gum disease and periodontal disease?
Gum disease (Gingivitis).
Characterized by bleeding gums.
Gum disease also known as Gingivitis is the inflammation of the marginal/outermost soft tissue surrounding a tooth.
Reversible.
Caused by presence of too much plaques (containing bacteria's) or by overly sensitive immune response to normal levels of plaques i.e. pregnancy.
Lack of immune response due to various systemic and/or environmental reasons, will lead to faster progression of disease, because the body's immune defence is not initiated.
Periodontal disease:
Progression of untreated gum disease such that irreversible damage is done to the mechanical barrier surrounding the tooth.
Inflammation has progressed to involve bone and periodontal ligaments.
Inflammatory process results in loss of bone surrounding the teeth, and produces pockets.
(photo of x-ray before/after).
This produces deeper spaces around the teeth referred to as ”pockets”.
Deeper portions of these pockets are not exposed to as much oxygen when we breathe, and can therefore provide environments for anaerobic bacteria's, which are much more harmful and destructive to periodontal tissues.
If not treated, leads to tooth mobility, and eventually tooth loss.
In addition, bacteria are more likely to enter our systemic circulation and lead to increased risk of systemic problems.
Treatment programs:
Gum disease (gingivitis)
Supragingival scaling and satisfactory home hygiene is enough.
Generally topical anaesthetics is sufficient , i.e. gels, sprays.
6 month intervals with your hygienist is recommended.
Periodontal disease:
Much more serious problem than gingivitis and requires multiple appointments to properly clean the deeper plaques from root surfaces.
Local anaesthesia required.
Multiple appointments are required to get under control, followed by 3 month maintenance cleaning.
If maintenance is not kept up, deeper cleanings are again required.
Treatment program by appointment (may vary for some cases).
Appointment 1: supragingival scaling (normal teeth clean).
Appointment 2&3: subgingival quadrant root planning (deep cleaning).
Appointment 4: review.
Follow up 3 month interval (normal teeth clean).
Diabetics, Smokers are at greater risk due to impaired blood circulation, and therefore impaired immune defence.
Genetics can play a big role in susceptibility to periodontal disease.
Patient maintenance instructions:
Three month interval hygienist visits.
Topical chlorhexidine based gels and mouthwashes.
Interdental brushes for approximal surface cleaning (cleaning between teeth).
Recession:
Loss of soft tissue exposing the root of the tooth.
The exposed root dentin is much softer than the enamel and has a more opaque yellow appearance.
Strong brushing of this yellow surface is a mistake and can lead to abrasion, weakening the tooth and increasing sensitivity.
Strong brushing with too hard of a toothbrush can also increase risk of recession by damaging the soft tissues.
Fluoride toothpastes and gentle tooth brushing are recommended to decrease sensitivity.
Concept:
Soft tissue is proportional to the underlying bone, primarily due to blood supply coming from the bone.
If we loose bone, we will loose soft tissue --> recession.
Loss of bone and therefore soft tissues can be either a natural phenomenon due to changes in bone density, or pathological - as in the case of periodontal disease.
Soft tissue is categorized as either thick biotype, or thin biotype.
Individuals with a thin biotype, are more susceptible to recession, as their tissue is more fragile.
The bone surrounding the outer surface of the teeth can be very thin towards the crest of the soft tissues, and this bone can be even thinner when crowding is present and teeth are pushed outwards In the bony arch.
Naturally as we age, the thinnest, sharpest portion of the surrounding bone will round out and therefore decrease in height around the tooth.
As a result, soft tissues will decrease as well, and recession occurs.